Of all the concerns that arise in conversations about testosterone replacement therapy, cardiovascular safety is the one that carries the most weight — and the most misinformation. Men are told that TRT and Cardiovascular Health are incompatible, and that TRT is dangerous for the heart. GPs often cite cardiovascular risk as a reason to decline or defer treatment. Headlines about testosterone and heart attacks circulate periodically. And yet many of these concerns are based on research that has been significantly reassessed, revised, or superseded by better evidence.
At Vitalis Luxe Clinic in Hull, we take cardiovascular safety seriously — it is at the core of how we prescribe and monitor TRT. We also take our responsibility to give men accurate information seriously. The evidence on TRT Cardiovascular VitalisLuxeand cardiovascular health is now substantially more reassuring than the coverage of a decade ago suggested — and men deserve to understand why.
This article reviews the full evidence base: the studies that raised concern, why those studies were problematic, what better-designed research has shown, what the genuine cardiovascular considerations of TRT are, and how they are managed in a properly supervised clinical programme.
Table of Contents
The Origin of the Cardiovascular Controversy
The 2013–2014 Studies That Created the Alarm

The cardiovascular concerns around TRT trace primarily to two observational studies published in 2013 and 2014. The first, by Vigen et al. (2013) in JAMA, reported increased rates of heart attack, stroke, and death in men on TRT who had undergone coronary angiography. The second, by Finkle et al. (2014) in PLOS ONE, reported increased rates of non-fatal heart attacks in the 90 days after TRT prescription in older men.
Both studies received extensive media coverage and prompted the US FDA and European regulatory authorities to issue label changes requiring cardiovascular risk warnings on TRT products. They appeared to confirm a long-standing theoretical concern that testosterone might promote cardiovascular disease.
Why Those Studies Were Critically Flawed

The Vigen et al. study was subsequently found to contain a significant data error: the original statistical analysis miscoded the outcomes of 100+ female patients as male — a fundamental methodological error that, when corrected, substantially changed the findings. The study’s comparison group was also problematic, and the methodology was subsequently critiqued extensively in peer-reviewed letters and reanalyses. A correction was issued but received far less media attention than the original paper.
The Finkle et al. study compared two groups that were not adequately matched — men receiving TRT versus men receiving PDE5 inhibitors (erectile dysfunction medications). The TRT group was substantially older and sicker at baseline, creating a confounding that was not adequately controlled. Men who are unwell enough to have sought treatment for low testosterone are not the same population as men seeking ED medication.
In the years since, multiple systematic reviews and meta-analyses of better-designed research have revisited the cardiovascular question — and reached very different conclusions.
What the Better Evidence Shows
Systematic Reviews and Meta-Analyses

A 2018 meta-analysis by Corona et al. — analysing 30 randomised controlled trials of TRT involving over 8,000 patients — found no statistically significant increase in major adverse cardiovascular events (MACE: heart attack, stroke, cardiovascular death) in men on TRT compared to placebo. A 2019 systematic review by Kaufman et al. similarly found no evidence of increased cardiovascular risk from TRT in properly conducted trials.
These analyses consistently note that the highest cardiovascular risk from TRT is associated with protocols that produce supraphysiological testosterone levels, that the risk profile of clinically appropriate TRT maintaining physiological levels is substantially different from anabolic steroid abuse, and that men with clinically confirmed hypogonadism may actually be at higher cardiovascular risk from their untreated deficiency than from properly monitored TRT.
The TRAVERSE Trial: The Largest RCT to Date

The most definitive evidence to date comes from the TRAVERSE trial (Testosterone Replacement Therapy for Assessment of Long-term Vascular Events and Efficacy ResponSE), published in the New England Journal of Medicine in 2023. TRAVERSE was a large, randomised, double-blind, placebo-controlled trial specifically designed to assess the cardiovascular safety of TRT in middle-aged and older men with hypogonadism and elevated cardiovascular risk.
The key finding: testosterone gel did not increase the rate of major adverse cardiovascular events (non-fatal heart attack, non-fatal stroke, or cardiovascular death) compared to placebo over a follow-up period of approximately 33 months. There was no statistically significant difference in MACE between the TRT and placebo groups.
The TRAVERSE trial did identify one area of concern: increased rates of atrial fibrillation and pulmonary embolism in the TRT group compared to placebo. These findings are important and inform how TRT is prescribed and monitored — but they do not support the conclusion that TRT broadly increases heart attack or stroke risk. They do support the importance of proper patient selection and monitoring.
The Cardiovascular Effects of Low Testosterone: The Other Side of the Equation
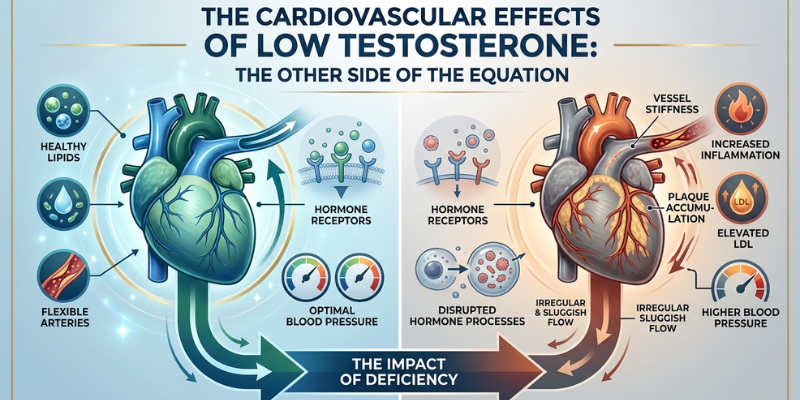
A critical dimension of the cardiovascular safety discussion that is often omitted: the cardiovascular consequences of untreated testosterone deficiency. The risk calculation is not TRT versus no risk — it is TRT versus the documented risks of chronic hypogonadism.
Cardiovascular Parameter | Effect of Low Testosterone | Effect of TRT Restoration |
|---|---|---|
Visceral adiposity | Significantly increased — promotes insulin resistance and atherogenic dyslipidaemia | Reduces visceral fat with sustained treatment; improves metabolic risk profile |
Insulin resistance / type 2 diabetes risk | Substantially elevated in hypogonadal men — bidirectional relationship with metabolic syndrome | TRT improves insulin sensitivity; reduces HbA1c in some studies of diabetic hypogonadal men |
Lipid profile | Mixed — low T associated with reduced HDL (‘good’ cholesterol) and increased triglycerides | TRT modestly reduces total cholesterol and LDL in some studies; HDL effects variable |
Endothelial function | Impaired in hypogonadal men — reduced nitric oxide production, increased arterial stiffness | TRT improves endothelial function and reduces arterial stiffness — documented in multiple trials |
Inflammatory markers (CRP, IL-6) | Elevated in testosterone deficiency — chronic low-grade inflammation | TRT reduces CRP and inflammatory cytokines in hypogonadal men |
Haematocrit / erythrocytosis | No haematocrit elevation from deficiency itself | TRT raises haematocrit — requires monitoring; can increase blood viscosity if uncontrolled |
Cardiovascular mortality | Multiple large observational studies associate low testosterone with increased cardiovascular mortality | Appropriately dosed TRT associated with reduced or neutral cardiovascular mortality in most large studies |
The pattern that emerges from the evidence is consistent: low testosterone is itself a cardiovascular risk state. The clustering of low testosterone with visceral obesity, insulin resistance, dyslipidaemia, hypertension, and endothelial dysfunction is not coincidental — the hormonal deficit drives many of these risk factors directly. Treating the deficiency with properly managed TRT addresses multiple cardiovascular risk factors simultaneously.
The Genuine Cardiovascular Considerations of TRT

Acknowledging that the catastrophist narrative around TRT and heart disease is not supported by the best current evidence does not mean TRT carries no cardiovascular considerations. Several real and manageable considerations deserve clear clinical attention:
1. Erythrocytosis and Blood Viscosity
The most important cardiovascular safety parameter to monitor on TRT is haematocrit — the proportion of blood volume that is red blood cells. TRT stimulates erythropoiesis (red blood cell production), and in a significant minority of men, haematocrit rises above the normal range (52%). Elevated haematocrit increases blood viscosity, which in theory increases the risk of thromboembolic events.
This risk is real but manageable with proper monitoring. At Vitalis Luxe Clinic, haematocrit is checked at 6–8 weeks, 3 months, and 6-monthly thereafter. If it rises to concerning levels, dose adjustment or therapeutic phlebotomy (removal of a unit of blood) rapidly normalises values. Men with baseline high-normal haematocrit, sleep apnoea, or significant dehydration are at higher risk and require closer monitoring.
2. Atrial Fibrillation
The TRAVERSE trial identified a modest but statistically significant increase in atrial fibrillation (AF) in the TRT group. The absolute numbers were small and the clinical significance in individual patients remains debated. However, this finding supports careful patient selection and monitoring — men with pre-existing AF or significant AF risk factors (older age, hypertension, obesity, sleep apnoea) should have this discussed explicitly before starting TRT.
3. Pulmonary Embolism
TRAVERSE also found a small increase in pulmonary embolism in the TRT group. The mechanism is likely related to erythrocytosis and increased blood viscosity rather than a direct thrombogenic effect of testosterone. The absolute risk remains low, but it reinforces the importance of haematocrit monitoring and dose optimisation.
4. Men with Pre-existing Cardiovascular Disease
For men with a history of recent myocardial infarction (within 6 months), significant heart failure, or severe aortic stenosis, TRT initiation requires specialist cardiology input and careful risk-benefit assessment. These are not absolute contraindications — the cardiovascular risk of untreated hypogonadism must be weighed against TRT risks — but they represent clinical situations requiring more than routine monitoring.
5. Supraphysiological Testosterone: The Separate Risk Profile
It is clinically essential to distinguish between clinically appropriate TRT that maintains testosterone in the physiological range and the supraphysiological doses used in anabolic steroid abuse. The cardiovascular harms of anabolic steroid abuse — left ventricular hypertrophy, hypertension, polycythaemia, adverse lipid profiles, and direct myocardial toxicity — are well-documented and severe. They are not representative of what properly dosed TRT produces. Equating them is a category error.
The Balanced Clinical View Clinically appropriate TRT in men with confirmed testosterone deficiency — maintained in the physiological range with regular haematocrit monitoring — does not appear to increase the risk of heart attack or stroke based on the best current evidence. It does carry a small increase in atrial fibrillation risk and a haematocrit-mediated thromboembolic consideration that are managed through proper clinical oversight. The cardiovascular risk of untreated testosterone deficiency — through visceral obesity, insulin resistance, endothelial dysfunction, and systemic inflammation — is also real and documented. For most men, the risk balance favours properly managed TRT over chronic untreated deficiency. |
TRT and the Cardiovascular Risk Assessment
At Vitalis Luxe Clinic, every man being assessed for TRT receives a baseline cardiovascular risk evaluation as standard — not as a barrier to treatment, but as the foundation of safe prescribing and monitoring. This assessment includes:
- Blood pressure measurement — hypertension is the most prevalent modifiable cardiovascular risk factor and interacts with erythrocytosis risk on TRT
- Fasting glucose and HbA1c — insulin resistance and diabetes are strongly associated with both testosterone deficiency and cardiovascular disease
- Fasting lipid profile — total cholesterol, HDL, LDL, and triglycerides; establishes baseline and identifies pre-existing dyslipidaemia
- Full blood count including haematocrit — baseline for the most important TRT safety parameter
- BMI and waist circumference — proxy measures of visceral adiposity and metabolic risk
- Cardiovascular history — past events, family history, current medications
- Smoking history and alcohol intake
- Sleep apnoea symptoms — sleep apnoea independently raises haematocrit, cardiovascular risk, and TRT-related complications
This is not bureaucracy — it is the clinical foundation that allows safe, effective TRT prescribing. Men who obtain testosterone without this baseline assessment are taking risks that proper clinical oversight prevents.
Frequently Asked Questions
Is TRT safe for men with heart disease?
For most men with stable, managed cardiovascular disease, properly monitored TRT is not contraindicated. The key qualifiers are ‘stable’ and ‘managed’ — men with a recent myocardial infarction (within 6 months), decompensated heart failure, or unstable angina require cardiology input before TRT initiation. For men with stable coronary artery disease, hypertension, or previous cardiac events who are well-managed, the cardiovascular benefits of treating confirmed testosterone deficiency often outweigh the risks. This is an individualised clinical assessment.
Does TRT cause heart attacks?
The best current evidence does not support the conclusion that clinically appropriate TRT — maintaining testosterone within the physiological range with regular monitoring — significantly increases the risk of heart attack or stroke. Early observational studies that raised this concern have been substantially critiqued for methodological flaws. The TRAVERSE trial — the largest and most rigorous RCT on TRT cardiovascular safety — found no increase in major adverse cardiovascular events. Anabolic steroid abuse at supraphysiological doses is a different and genuinely dangerous category.
What did the TRAVERSE trial find about TRT and heart safety?
TRAVERSE was a large randomised controlled trial specifically designed to assess TRT cardiovascular safety in high-risk men. It found no increase in the composite rate of non-fatal heart attack, non-fatal stroke, or cardiovascular death in the TRT group compared to placebo. It did identify modest increases in atrial fibrillation and pulmonary embolism — findings that inform monitoring practice but do not establish broad cardiovascular harm from TRT.
Does low testosterone increase heart disease risk?
Yes — multiple large observational studies associate low testosterone with increased cardiovascular mortality, independently of traditional cardiovascular risk factors. Low testosterone is mechanistically linked to visceral adiposity, insulin resistance, endothelial dysfunction, adverse lipid profiles, and systemic inflammation — all of which increase cardiovascular risk. The risk calculation for TRT is not ‘TRT risk vs. zero risk’ but ‘TRT risk vs. the documented cardiovascular risk of untreated testosterone deficiency.’
How does TRT affect blood clotting risk?
The primary mechanism through which TRT may affect clotting risk is erythrocytosis — elevated red blood cell count increasing blood viscosity. This is monitored through regular haematocrit checks at every blood test. If haematocrit rises significantly, dose reduction or phlebotomy normalises it. The absolute risk of thromboembolic events in properly monitored TRT is low. Men with a personal or family history of deep vein thrombosis or pulmonary embolism should disclose this at their clinical assessment.
Is TRT safe if I have high blood pressure?
Hypertension is common in men with testosterone deficiency, partly because of the metabolic effects of deficiency itself. TRT in men with well-controlled hypertension — on appropriate antihypertensive medication — is generally manageable. Blood pressure is monitored at every clinic review. TRT may modestly improve blood pressure in some men through its metabolic effects. Men with severe, uncontrolled hypertension should address blood pressure control before or simultaneously with TRT initiation.
What cardiovascular tests should I have before TRT?
At a minimum: blood pressure, fasting glucose or HbA1c, fasting lipid profile, full blood count including haematocrit, and ECG in men with significant cardiovascular history or symptoms. A cardiovascular history covering past events, family history, smoking, alcohol intake, and sleep apnoea symptoms completes the baseline assessment. At Vitalis Luxe Clinic in Hull, all of these are incorporated into the comprehensive pre-TRT assessment as standard.
Where can I get TRT safely managed in Hull or Yorkshire?
Vitalis Luxe Clinic provides clinician-led TRT with comprehensive cardiovascular baseline assessment and ongoing monitoring for men across Hull, East Yorkshire, and throughout Yorkshire. Our approach is built on the current evidence — neither dismissing genuine considerations nor overstating risks that the evidence does not support. In-person at our Hull clinic or online with home testing — no GP referral required.
The Evidence Is Clearer Than the Headlines Suggested
The cardiovascular alarm around TRT was based on flawed studies that have since been substantially revised by better evidence. The TRAVERSE trial and multiple meta-analyses give a far more reassuring picture for men with confirmed deficiency who are properly monitored. The genuine cardiovascular considerations of TRT — erythrocytosis, atrial fibrillation risk, haematocrit monitoring — are real and are managed through appropriate clinical oversight. They are not reasons to deny men with confirmed testosterone deficiency the treatment they need. At Vitalis Luxe Clinic in Hull, we prescribe TRT on the basis of the current evidence — with rigorous monitoring, honest communication, and the cardiovascular assessment that safe prescribing requires. Serving men across Hull, East Yorkshire, and throughout Yorkshire. |